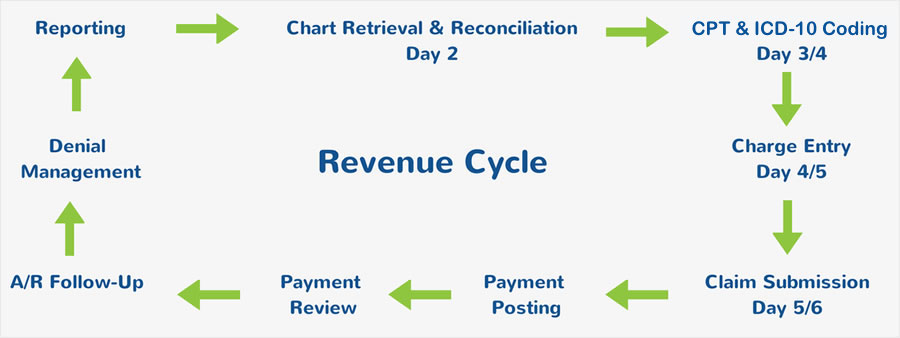
Our medical billing and claims management services are designed to optimize the billing and collection cycle with compliance-focused policies and procedures ensuring you receive proper compensation for services provided.
What We Offer
- Comprehensive revenue cycle service
- Patient billing and inquiry management
- Comprehensive productivity and financial reporting
- Customized data mining and reporting
- Compliance-focused policies and procedures
- Competitive pricing

What You Can Expect
Value-Added Services
- 100% chart reconciliation
- Accurate and compliant coding practice
- Provider documentation, education and feedback
- Aggressive revenue cycle management
- Assist with third-party payer negotiations
- Established knowledge base in emergency medicine

Free Chart Audit & Billing Analysis
Our free chart review and revenue forecast analysis offers the results you could expect from PBS if we were to handle your billing needs. Contact us today online or at 937-436-4658 x201.
Contact Us